It’s not exactly a secret that America’s heroin epidemic has spiraled out of control in recent years.
According to one 2015 study, there are almost 1 million Americans abusing heroin on an annual basis. The problem has gotten to be so bad that some states like Pennsylvania and Florida have declared a state of emergency over it.
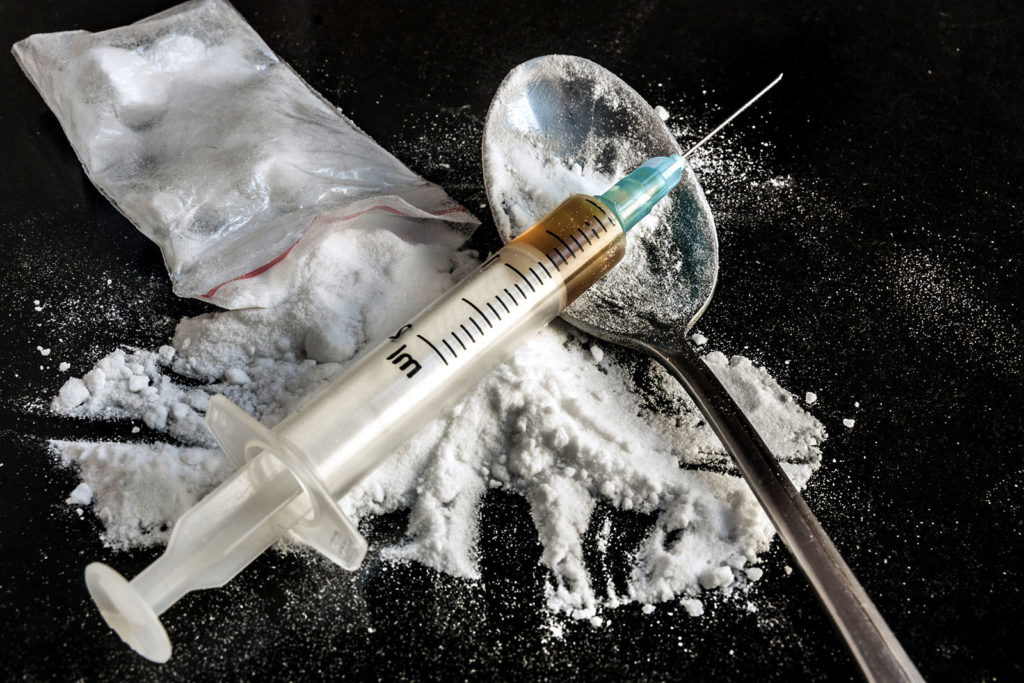
What Is Heroin?
This drug exists in several different forms. Most commonly, heroin comes in the form of either a white or brown powder. But in some instances, heroin will also take the form of a black substance that’s very sticky. This form of heroin is commonly called black tar heroin.
Definition
Heroin is an opioid drug that is manufactured from morphine. The morphine that is used to make heroin originates from poppy plants that are most often found in places like Mexico, Colombia, and different parts of Asia.
How Is It Taken?
There are a few ways in which heroin users will use the drug. People can inject heroin, snort it, sniff it, and smoke it. There are also people who choose to mix heroin together with crack cocaine before injecting or snorting it as part of a dangerous practice that is called speedballing.
Who Takes It?
One of the reasons why heroin has turned into such a big issue in America is because it’s abused by those of almost all ages at a high rate. But the increase in heroin use in the U.S. as a whole appears to be closely tied to the increase in heroin use in those who fall between the ages of 18 and 25.
This helps explains why the number of people trying heroin for the very first time spiked from 90,000 people in 2007 to 170,000 people in 2016.
Recovery is One Phone Call Away
You deserve to live a life free from the grips of addiction. Contact us today to learn how to find the right GET HELP NOW for you!
GET HELP NOWA Brief History of Heroin
Despite the recent surge of heroin users, heroin is not a particularly new drug. It was first synthesized from morphine way back in the 1870s and was sold commercially in the late 1890s by the Bayer Pharmaceutical Company. It was, at one time, thought to be a worthy replacement to the highly-addictive morphine.
However, heroin was eventually outlawed in the U.S. and many other parts of the world after it was found to be every bit as addictive and dangerous as morphine.
Consequences of Heroin Use
Heroin has become one of the most abused drugs in the U.S. and on the planet as a whole because of the effects that it has on both the mind and the body. The so-called “heroin high” is unlike almost any other high associated with using drugs.
Effects on the Mind and Body
Heroin can cause a variety of effects for those who choose to use it. A few of those effects are listed below:
- Binds to the opioid receptors located in a person’s brains within just a few seconds and produces an almost instant feeling of euphoria due to a sudden increase in dopamine levels
- Knocks out unpleasant feelings of depression and anxiety and makes a person feel happier than they would feel otherwise with their life
- Creates feelings of warmth and even safety and makes those who might be in a dangerous situation feel secure in their surroundings
- Eliminates any physical pain that a person might be feeling in the various parts of their body
- Slows down a person’s heart rate and breathing and brings down their blood pressure
A “heroin high” will usually take hold of a person and impact their mind and body very quickly. But it also doesn’t take long to wear off. More often than not, the high produced by using heroin will only last for a few minutes before a person begins to come down from it.
From there, there are many short- and long-term health effects associated with heroin use. They range from relatively minor inconveniences to extremely serious health complications.
Are You Ready to Get Help?
Our treatment specialists are available 24/7 to help you or your loved one find a treatment program that suits your needs. It only takes one call to start your new life in recovery!
GET HELP NOWShort-Term Health Effects
When a person first uses heroin, they usually won’t feel anything other than the euphoria that comes along with it. But shortly after that, there are short-term health effects that will start to set in. They include:
- Dry mouth
- A heavy feeling that takes over both the arms and the legs
- Warm flushing of a person’s skin
- Nausea
- Vomiting
- An inability to think clearly
- Moderate to severe itching
Some of these short-term health effects will disappear once the heroin makes its way out of a person’s system. But some of them will linger and, in some cases, even get worse once the heroin is gone.
Long-Term Health Effects
In addition to short-term health effects, a person can also face many long-term health effects when using heroin regularly. They include:
- Insomnia
- An infection in the lining of the heart
- Swollen pus-filled tissues called abscesses in different areas of the body
- Constipation
- Severe stomach cramping
- Kidney disease
- Liver disease
- Lung diseases
- Depression
Many heroin users also share needles to inject heroin. By doing this, they increase the chances of contracting serious diseases like hepatitis and HIV.
Additionally, those who use heroin can overdose on the drug and die if they take too much of it at once. There were more than 70,000 people who overdosed on heroin and other illicit drugs in 2017 alone.
Questions About Treatment?
If you or your loved one is struggling with addiction, you probably have many questions regarding your options for treatment. Our admissions counselors are standing by to answer your questions!
GET HELP NOWUsing Heroin With Other Drugs
Studies have shown that the majority of the people who use heroin use at least one other drug, too.
Which Drugs Are Commonly Used With Heroin?
As previously mentioned, there are some heroin users who will mix the drug with cocaine to create a concoction called “speedball.” There are also heroin users who drink alcohol while under the influence of heroin.
Some heroin users will even mix the drug with benzodiazepines, including drugs like Valium, Xanax, and more. This is especially dangerous because both heroin and benzodiazepines can slow down your breathing dramatically and put your body at risk. The combination of the two can also stop naloxone, a drug that’s used to reverse an overdose, from doing its job.
How much does Heroin cost?
Some people seek out heroin as a way to get a cheaper alternative to prescription opioid painkillers. The lower cost of heroin and the high availability make it a drug of choice for many people. The biggest problem is that the considerable cost of heroin doesn’t usually hit until the person is addicted to it. The daily hits, along with the enormous costs personally and professionally, add up quickly.
The Street Cost
How much does heroin cost on the street? This price usually varies depending on where you are in the world. On average, heroin costs between $5 to $10 for a small bag. These little wax paper or plastic bags usually have about 1/10 of a gram in them. In bigger cities, this cost can jump up to $20 per bag. An 80-milligram OxyContin tablet goes for about $80 on the street. A 15 to 30-milligram tablet goes for about $30. This means heroine is a much smaller cost for the same amount of high. This drug is highly addictive so that the person will need more and more over time. They might end up spending hundreds of dollars a day to get their fix.
The Factors
Heroin is less expensive than prescription opioids, but the price often fluctuates. The type of heroin the person wants is one of the most significant factors regarding price. Supply and demand also take place in the sale. The cut and processing of heroin is also a significant factor. The purer the heroin, the more expensive it is. Though the seller may state it’s pure, it could be laced with other substances. Price isn’t always genuine when it comes to drugs on the street.
The Cheap Drug Reasoning
As stated before, the price of heroin often depends on where it is sold. Drug cartels also watched the most significant sales in specific regions and pumped up their volume for more money. They create new networks and new production areas so they can fill the need for heroin users who think opioid pills are too expensive. The demand is so high that the supply flows smoothly. This is an easy way to keep the price low while maintaining high production. Drugs like OxyContin have gotten harder for many people to get and share. Instead of stopping the drug, many turn to heroin because it’s easier and cheaper to get.
Ease Of Use
Heroin is easier to use than pills. Prescription painkillers now often come in extended low doses. This means the person abusing the pills would have to crush them, then snort or inject them. Most painkillers are now harder to crush. They also aren’t easy to dissolve, meaning it’s hard to inject them. Heroin is easier to get a fast high. It comes in a very fine powder or as a tarlike substance. It’s ready in a few minutes.
How much does heroin cost in the end? It adds up to be a costly drug. At first, the person is paying much less than prescription painkillers. In the end, the person is paying between $50,000 and $100,000 a year to reach their high. The price and availability of the drug are leading to overdoses and death throughout the world. The negative impact it has on those that use it is priceless.
Treating Heroin Addiction
If you or someone you know struggle with heroin addiction, you can get the help you need to kick your habit. It’ll help you avoid the short-term and long-term health effects associated with it and allow you to live a happier, healthier life.
Get started by taking a look at what kind of detox programs and treatment options your insurance company might cover.

